By Gaelyn Lyons
At some point in our lives, we will get the dreaded news that we need to get an aching tooth filled, a suspicious mole biopsied, or a stoned gallbladder surgically removed. Thanks to modern medicine, we can get through all these procedures somewhat painlessly with the help of anesthesia. Contrary to popular belief, anesthesia is much more than just sedating patients for major surgery. Anesthesia is a type of treatment that is done to prevent pain during medical procedures, and the medications that are given to achieve pain management are called anesthetics.1 Depending on the type of anesthesia that is being administered, a patient can become numb or lose consciousness. Some common procedures that are performed with the assistance of anesthesia are tooth fillings or extractions, childbirth, colonoscopies, and surgeries.2 There are many ways in which anesthesia can be administered, including intramuscular (similar to your annual flu shot) or intravenous injections, inhalation of gas, or topical application.1
The History of Modern Anesthesia
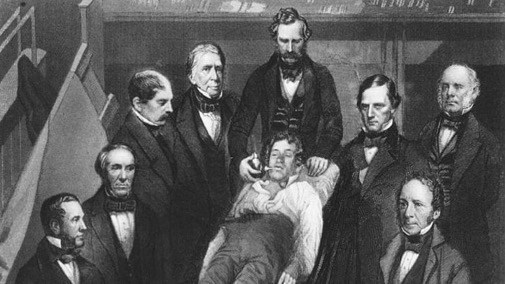
Prior to the introduction of using anesthesia, surgery was only performed as a last resort because of the traumatic nature of a patient being fully aware during the procedure.3 However, when surgery was being done, the best a surgeon could offer their patients were opium, alcohol, or something to bite on.4 It wasn’t until the first public demonstration of surgery using anesthesia on October 16, 1848 that physicians took the use of anesthesia seriously.4,5 Anesthesiologist Dr. William T.G. Morton, along with surgeon John Collins Warren, demonstrated that the use of sulfuric ether was just as safe and effective at providing pain relief as the nitric oxide that was being used at the time (Figure 1).4,6 Once word of the successful surgery got out, anesthesia became more widely used and allowed for surgeons take their time and access parts of the body that were basically impossible to work on before.7 This groundbreaking achievement began the evolution of using other anesthetics like chloroform, nitrous oxide, and cocaine during painful procedures like childbirth, tooth extractions, and surgeries.5
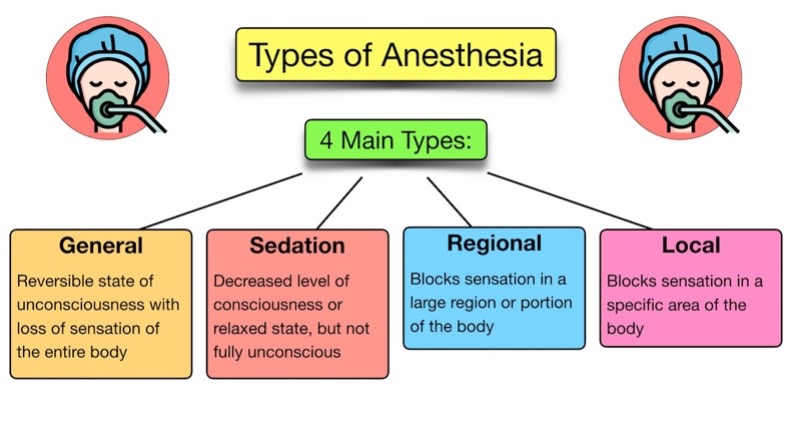
Fortunately, scientists and surgeons have developed more evolved anesthetics that are better at pain management, more reliable at inducing loss of consciousness, and much safer. Today, there are four major types of anesthesia that are used: local anesthesia, regional anesthesia, sedation, and general anesthesia (Figure 2).8–10
Local Anesthesia
Local anesthesia is used to numb a small part of the body or to help manage pain during or after a surgery or procedure.8,11 The anesthetic can be administered through an injection, gel, or ointment, and the procedure is often done while the patient is awake.11,12 Common procedures that utilize local anesthesia include skin biopsies, stitching deep wounds, and tooth fillings or extractions. Local anesthesia works by preventing nerves from sending pain signals to the brain. The most common local anesthetic that is used is lidocaine.
Regional Anesthesia
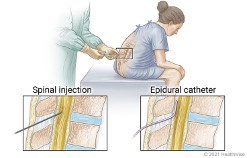
Regional anesthesia involves injecting an anesthetic near a group of nerves to numb a larger area of the body and is often used during orthopedic surgeries, bladder and urinary tract surgeries, and reproductive procedures.13 The most frequently used types of regional anesthesia are spinal anesthesia and epidural anesthesia.14 Spinal anesthesia is administered by placing a needle into the subarachnoid space of the spine and injecting a local anesthetic medication into the cerebral spinal fluid (CSF).13,15 The needle is removed as soon as the anesthetic is injected into the CSF.14 Epidural anesthesia is similar to spinal anesthesia; however, the anesthetic is injected into the epidural space through a catheter that remains in the patient to allow for long-term administration (Figure 3).14,15 Spinal anesthesia is commonly used for surgeries on the lower part of the body while epidural anesthesia is commonly used during labor and childbirth.16
Peripheral nerve blocks are another type of regional anesthesia that are commonly used for pain relief and prevention of movement during procedures. Anesthetics are injected into a bundle of nerves closest to the area being operated on.14
Monitored Anesthesia Care
Monitored anesthesia care, also referred to as sedation, is a method of anesthetic administration that is monitored by a clinician known as an anesthesiologist.17 The three main focuses of monitored anesthesia care are to provide a safe level of sedation, alleviate any patient anxiety, and provide adequate pain relief.18 Depending on the procedure being done, a patient may be sedated at different levels. When minimally sedated, a patient is awake and able to interact with their surgeon.19,20 When moderately sedated, a patient is drowsy and might even fall asleep; however, they are easily aroused.18–20 When under deep sedation, the patient is still conscious, but may be unaware of their surroundings.18–20 Some procedures that are done while sedated include endoscopies for gastroenterology issues, minor surgeries, and bone realignment to fix a broken bone.21
General Anesthesia
General anesthesia is often used during major surgeries. Similarly, to the previously mentioned anesthetic types, the purpose of general anesthesia is to provide pain relief to a patient while undergoing surgery. However, under general anesthesia, the patient is completely unconscious and is unable to move.22,23 General anesthesia is administered to the patient either through intravenous injection or inhalation of a gas through a breathing mask.24
While molecular mechanisms of pain management and anesthesia have been studied by many, the overall mechanism of how general anesthesia induces unconsciousness is still unknown. Many anesthetics increase the activation of gamma-aminobutyric acid (GABA) receptors, which are receptors that neuronal activity.25,26 When bound by their ligand or a drug that induces their activation, GABA receptors inhibit nerve transmission.27 Since inhibition of neuron activity would affect the whole brain, it is proposed that anesthesia potentially affects the connection between the regions of the brain that play a role in consciousness, specifically the cerebral cortex, thalamus, brainstem, and basal forebrain.26
Modern medicine has benefitted greatly from the introduction of anesthesia. Each type of anesthesia allows physicians to adequately treat their patients depending on their level of comfort, the duration of a procedure, and the invasiveness of a procedure. Without anesthesia, surgeries would be much more burdensome, not only for the surgeons, but also those who go under the knife. In addition to alleviating physical pain, anesthesia can alleviate the mental pain and anxiety that comes along with the fear of having surgery.
TL:DR
- Before the routine use of anesthesia during medical procedures, patients were given opium, alcohol, or something to bite on.
- There are four types of anesthesia: local anesthesia, regional anesthesia, monitored anesthesia care (sedation), and general anesthesia.
- The mechanism in which anesthesia induces unconsciousness is still unknown.
References
- Anesthesia: Anesthesiology, Surgery, Side Effects, Types, Risk. Cleveland Clinic https://my.clevelandclinic.org/health/treatments/15286-anesthesia (2020).
- Anesthesia. MedlinePlus https://medlineplus.gov/anesthesia.html#:~:text=What is anesthesia%3F,loss of feeling or awareness (2020).
- How agonising surgery paved the way for anaesthetics – BBC Future. https://www.bbc.com/future/article/20200624-how-agonising-surgery-paved-the-way-for-anaesthetics.
- Harrah, S. Medical Milestones: Discovery of Anesthesia and Timeline. University of Medicine and Health Sciences https://www.umhs-sk.org/blog/medical-milestones-discovery-anesthesia-timeline (2015).
- History of Anesthesia – Wood Library-Museum of Anesthesiology. https://www.woodlibrarymuseum.org/history-of-anesthesia/.
- Robinson, D. H. & Toledo, A. H. Historical Development of Modern Anesthesia. http://dx.doi.org/10.3109/08941939.2012.690328 25, 141–149 (2012).
- History of Anesthesia. World Federation of Societies of Anesthesiologists https://wfsahq.org/about/history/history-of-anaesthesia/.
- Types of Anesthesia. UCLA Health https://www.uclahealth.org/medical-services/anesthesiology/types-anesthesia#:~:text=There are four main categories,%22)%2C and local anesthesia.
- Local Anesthesia. American Society of Anesthesiologists https://www.asahq.org/madeforthismoment/anesthesia-101/types-of-anesthesia/local-anesthesia/#:~:text=Local anesthesia%2C also called local,or stitching a deep cut.
- General Anesthesia vs Sedation: Definition, Drugs, Side Effects, List of Example Medications Used — EZmed. https://www.ezmedlearning.com/blog/general-anesthesia-sedation-drugs-definitions.
- Local anaesthesia – NHS. https://www.nhs.uk/conditions/local-anaesthesia/.
- Nordqvist, J. What is local anesthesia, what is it used for, and what are common side effects? MedicalNewToday https://www.medicalnewstoday.com/articles/265689 (2022).
- Torpy, J. M., Lynm, C. & Golub, R. M. Regional Anesthesia. JAMA 306, 781–781 (2011).
- Regional Anesthesia. https://www.bcm.edu/healthcare/specialties/anesthesia/regional-anesthesia.
- Spinal and Epidural Anesthesia Behavioral Health & Intellectual disAbility Services – Philadelphia, Pennsylvania. https://philadelphia.pa.networkofcare.org/mh/library/article.aspx?hwid=acl7147.
- Spinal and epidural anesthesia. MedlinePlus https://medlineplus.gov/ency/article/007413.htm#:~:text=Spinal anesthesia is often used,painful without any pain medicine. (2021).
- Rosero, E. Monitored anesthesia care in adults. UpToDate https://www.uptodate.com/contents/monitored-anesthesia-care-in-adults#:~:text=Monitored anesthesia care (MAC) is,converts to general anesthesia if (2022).
- Das, S. & Ghosh, S. Monitored anesthesia care: An overview. J. Anaesthesiol. Clin. Pharmacol. 31, 27 (2015).
- Types of Anesthesia Care | Department of Anesthesiology. https://anesthesiology.weill.cornell.edu/patients/types-anesthesia.
- IV/Monitored Sedation. American Society of Anesthesiologists https://www.asahq.org/madeforthismoment/anesthesia-101/types-of-anesthesia/ivmonitored-sedation/.
- Procedural Sedation | Johns Hopkins Medicine. https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/procedural-sedation.
- General Anesthesia. NHS https://www.nhs.uk/conditions/general-anaesthesia/ (2021).
- Smith, G., D’Cruz, J. R., Rondeau, B. & Goldman, J. General Anesthesia for Surgeons. StatPearls (2023).
- Anesthesia | Johns Hopkins Medicine. https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/types-of-anesthesia-and-your-anesthesiologist.
- Diao, S., Ni, J., Shi, X., Liu, P. & Xia, W. Mechanisms of action of general anesthetics. Front. Biosci. (Landmark Ed. 19, 747–757 (2014).
- Shin, T. J., Kim, P. J. & Choi, B. How general anesthetics work: from the perspective of reorganized connections within the brain. Korean J. Anesthesiol. 75, 124 (2022).
- Allen, M. J., Sabir, S. & Sharma, S. GABA Receptor. Trends Pharmacol. Sci. 2, 62–64 (2023).
I stayed awake all the way till the end. I LOVE SCIENCE HUMOR. But you knew that. Keep up the good work. I will share this. You are among the last students who will reach great heights.