By Mariam Melkumyan
Burnout is unfortunately a common feeling among graduate students. While you can find information on ways to fight burnout in a 2019 LTS article, in this piece, I intend to dive deeper and examine the neuroscience behind burnout.
First, as a quick reminder of the definition of burnout:
Burnout is a process of psychological reaction to long-term work-related stress1. The ICD-11, the international version of the DMS-5 and the standard for the recording and reporting of illnesses globally, describes burnout as a syndrome resulting from chronic workplace stress that has not been successfully managed2. According to the ICD-11, three identifying characteristics of burnout are:
- Feelings of energy depletion or exhaustion;
- Increased mental distance from one’s job, or feelings of negativism or cynicism related to one’s job;
- A sense of ineffectiveness or lack of accomplishment.
Inclusion of burnout in the ICD-11 means that burnout is now recognized as a psychological issue. However, do we understand the neuroscience behind burnout?
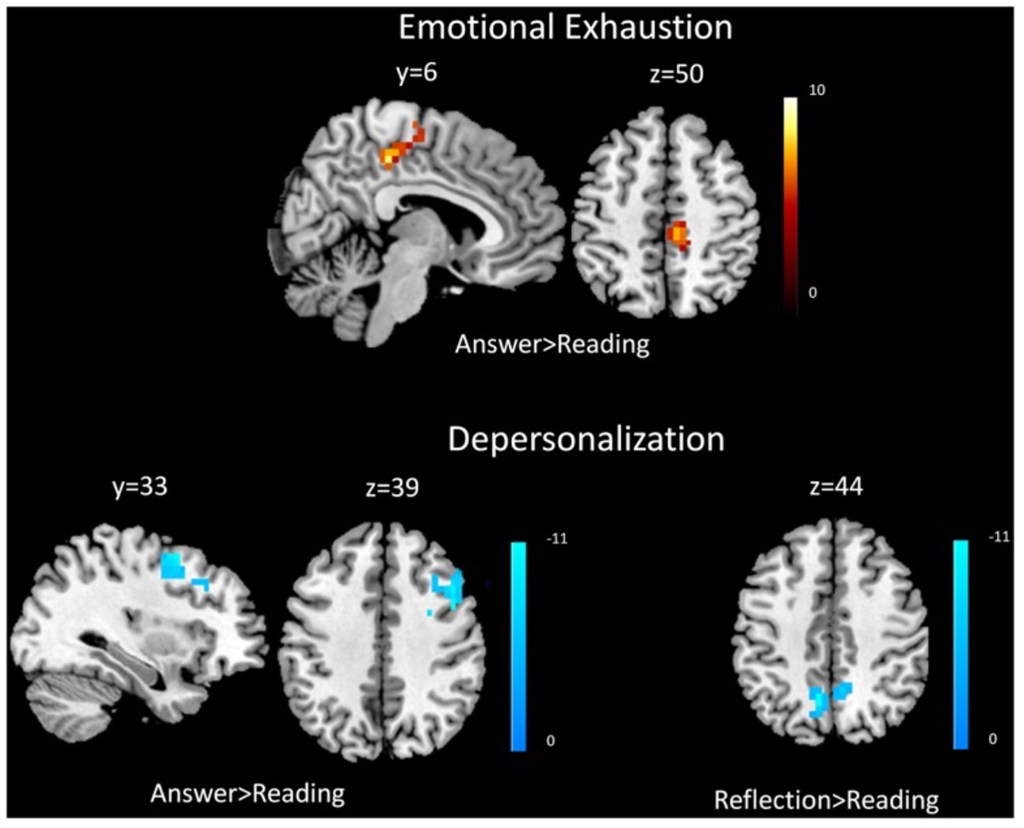
Chronic stress can cause a myriad of problems, both in the brain and the body. A study in 2011 tested the effect of chronic stress on serotonin receptor changes in the limbic networks. Serotonin is a neurotransmitter implicated in disorders such as depression and anxiety, and the limbic areas are highly involved in reward processing, regulation of the canonical stress axis, fear and anxiety, memory processing, attention, and emotion. The study found that with chronic psychosocial stress, the limbic region networks became dysfunctional. Furthermore, chronic stress led to a functional disconnection between the amygdala, a brain region important for processing fear and anxiety, and the medial prefrontal cortex, a brain region important for top-down control of the amygdala. The researchers also found that chronic stress reduced serotonin activity in areas important for attention and memory (anterior cingulate cortex and hippocampus). Overall, the study showed that chronic stress results in changes in brain activity, leading to issues in emotional and cognitive processing. Looking at burnout specifically, a study in 2013 used functional neuroimaging to explore the link between burnout and brain activity in medical residents and board-certified faculty3. The study found that individuals experiencing burnout had reduced activity in various brain regions important for cognitive processing, emotional processing3. Medical residents with burnout also had increased cognitive load and increased emotional exhaustion, leading to limited processing space and inefficient brain activation (Figure 1)3. Even though both faculty and medical residents experienced burnout, medical residents experiencing burnout had significant correlations between burnout and changes in brain activation, while the faculty did not3. Medical residents also had higher emotional exhaustion and depersonalization (feeling of observing yourself from outside of your body) – key components of burnout among physicians – scores, suggesting that residents need more cognitive and emotional support.
Another research article in 2013 tested the role of perceived chronic occupational stress on the brain volume, and found reductions in the anterior cingulate cortex, prefrontal cortex, and basal ganglia, areas sensitive to stress stimuli and involved in stress physiology4. Interestingly, these regions are similarly affected in combat veterans suffering from post-traumatic stress disorder, a striking parallel that emphasizes the importance of reducing occupational stress to avoid burnout. It is worth noting that in a resting state, when no task is being completed, individuals experiencing burnout may have cortical hyperactivity, which may be a compensatory mechanism related to increased mental effort1. If you have ever experienced burnout, this hyperactivity may be felt like your brain is (metaphorically) on fire (Figure 2), as thoughts race through your head with no direction. Other studies found increases in the volume of the amygdala5 associated with cases of burnout. This increase in the amygdala volume is correlated with severe stress in animal models6, a precedent that lends further credence to the other studies’ findings of disrupted stress mechanisms in people experiencing burnout.
The neuroscience behind burnout is actively being explored, and the number of studies exploring burnout in both the general population as well as student-specific groups is rising. Most research on burnout focuses on medical students and residents; however, there has been in increase in the number of studies exploring burnout in graduate students in the past few years. Several of these studies found that high levels of stress, anxiety, and depression symptoms were associated with increased levels of burnout in graduate students7. Research has found, notably, that good relationships with the advisor and advisor support reduced the risk of burnout. If you are feeling burnt out, reach out to talk or seek advice from friends, family, co-workers, your advisor, or anyone else that you may be comfortable with talking. Try to be mindful of your emotions and take a break from work. The Office for Professional Mental Health here at the College of Medicine has amazing resources and therapists who will support you, so don’t hesitate to reach out. Remember that your mental health is more important than any experiments! Take care of yourself and your brain will thank you!
TL:DR
- Multiple brain regions are involved in burnout, including regions involved in reward processing, stress axis, emotion, and attention
- Burnout may lead to cortical hyperactivity, making you feel like your brain is on fire
- If you are feeling burnt out, talk to friends, family, advisors, or licensed professionals to reduce your stress.
References
1. Golonka K, Gawlowska M, Mojsa-Kaja J, Marek T. Psychophysiological Characteristics of Burnout Syndrome: Resting-State EEG Analysis. Biomed Res Int. 2019;2019:3764354. doi:10.1155/2019/3764354
2. ICD-11 for Mortality and Morbidity Statistics. Accessed January 16, 2023. https://icd.who.int/browse11/l-m/en#/http://id.who.int/icd/entity/129180281
3. Durning SJ, Costanzo M, Artino AR, et al. Functional Neuroimaging Correlates of Burnout among Internal Medicine Residents and Faculty Members. Front Psychiatry. 2013;4:131. doi:10.3389/fpsyt.2013.00131
4. Blix E, Perski A, Berglund H, Savic I. Long-Term Occupational Stress Is Associated with Regional Reductions in Brain Tissue Volumes. PLoS One. 2013;8(6):e64065. doi:10.1371/journal.pone.0064065
5. Savic I. Structural changes of the brain in relation to occupational stress. Cereb Cortex. 2015;25(6):1554-1564. doi:10.1093/cercor/bht348
6. Boyle LM. A Neuroplasticity Hypothesis of Chronic Stress in the Basolateral Amygdala. Yale J Biol Med. 2013;86(2):117-125.
7. Allen HK, Lilly F, Green KM, Zanjani F, Vincent KB, Arria AM. Graduate student burnout: Substance use, mental health, and the moderating role of advisor satisfaction. Int J Ment Health Addict. 2022;20(2):1130-1146. doi:10.1007/s11469-020-00431-9.
8. Burki, Talha. How do you deal with burnout in the clinical workplace? The Lancet Respiratory Medicine. DOI:https://doi.org/10.1016/S2213-2600(15)00287-8.

Pingback: Get on the write track for an LTS blog post | Lions Talk Science